My Sick Liver
- Home
- Liver Functions
- Know Your Liver
- — Doctor's Visits
- — Lab Work
- — Imaging Tests
- — Liver Biopsies
- — Endoscopic Tests
- Liver Disease Information
- — Types
- — Stages
- — Measures
- — Complications
- — What Else To Do
- Liver Transplantation
- Organ/Tissue Donation
- Caregivers, Families & Friends
-
Miscellanea
- Newsletter
- Blog
- Contact Us
Autoimmune Liver Diseases
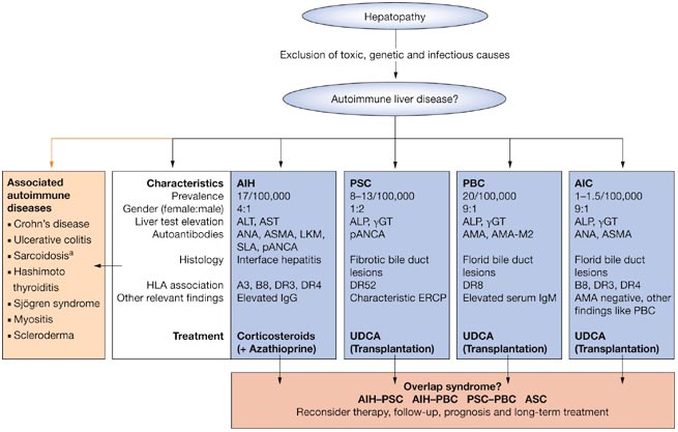
_Autoimmune hepatitis is inflammation in your liver that occurs when your body's immune system attacks your liver. Although the cause of autoimmune hepatitis isn't entirely clear, some diseases, toxins and drugs may trigger autoimmune hepatitis in susceptible people, especially women. Untreated autoimmune hepatitis can lead to scarring of the liver (cirrhosis) and eventually to liver failure. When diagnosed and treated early, however, autoimmune hepatitis often can be controlled with drugs that suppress the immune system. A liver transplant may be an option when autoimmune hepatitis doesn't respond to drug treatments or when liver disease is advanced.
Types of autoimmune hepatitis
Doctors have identified two main forms of autoimmune hepatitis:
The following is a list of examples of autoimmune disorders that may cause cirrhosis:
What are autoimmune disorders?
Autoimmune disorders are diseases that occur when the body produces an inappropriate immune response against its own tissues. Sometimes the immune system will cease to recognize one or more of the body's normal constituents as "self" and will produce auto antibodies – antibodies that attack its own cells, tissues, and/or organs. This causes inflammation and damage and leads to autoimmune disorders.
The cause of autoimmune diseases is unknown, but it appears that there is an inherited predisposition in many cases. In a few types of autoimmune disease (such as rheumatic fever), a virus or infection with bacteria triggers an immune response and the antibodies or T-cells attack normal cells because some part of their structure resembles a part of the infecting microorganism.
Autoimmune disorders fall into two general categories: those that damage many organs (systemic autoimmune diseases) and those where only a single organ or tissue is directly damaged by the autoimmune process (localized). However, the distinctions become blurred as the effect of localized autoimmune disorders frequently extends beyond the targeted tissues, indirectly affecting other body organs and systems.
Causes of Autoimmune Hepatitis
Autoimmune hepatitis occurs when the body's immune system, which ordinarily attacks viruses, bacteria and other pathogens, instead targets the liver. This attack on your liver can lead to chronic inflammation and serious damage to liver cells. Just why the body turns against itself is unclear, but researchers think autoimmune hepatitis could be caused by an interaction between several risk factors, such as infections, medications and a genetic predisposition.
Risk factors
Factors that may increase your risk of autoimmune hepatitis include:
Signs and symptoms of autoimmune hepatitis can range from minor to severe and may come on suddenly or develop over time. Some people have few, if any, problems in the early stages of the disease, whereas others experience signs and symptoms that may include:
Make an appointment with your doctor if you have any signs or symptoms that worry you.
Complications
Autoimmune hepatitis may be associated with a variety of other autoimmune diseases, including:
Tests and diagnosis
Tests and procedures used to diagnose autoimmune hepatitis include:
The goal in treating autoimmune hepatitis is to slow or stop your body's immune system from attacking your liver. This may help slow the progress of the disease. Medications to control your immune system (immunosuppressants) Medications used to treat autoimmune hepatitis include:
Types of autoimmune hepatitis
Doctors have identified two main forms of autoimmune hepatitis:
- Type 1 (classic) autoimmune hepatitis Often developing suddenly, this is the most common type of the disease. It can occur at any age. About half the people with type 1 autoimmune hepatitis have other autoimmune disorders, such as thyroiditis, rheumatoid arthritis or ulcerative colitis.
- Type 2 autoimmune hepatitis Although adults can develop type 2 autoimmune hepatitis, it's most common in young girls and often occurs with other autoimmune problems.
The following is a list of examples of autoimmune disorders that may cause cirrhosis:
- Autoimmune Hepatitis
- Primary Biliary Cirrhosis (PBC)
- Primary Sclerosing cholangitis (PSC)
What are autoimmune disorders?
Autoimmune disorders are diseases that occur when the body produces an inappropriate immune response against its own tissues. Sometimes the immune system will cease to recognize one or more of the body's normal constituents as "self" and will produce auto antibodies – antibodies that attack its own cells, tissues, and/or organs. This causes inflammation and damage and leads to autoimmune disorders.
The cause of autoimmune diseases is unknown, but it appears that there is an inherited predisposition in many cases. In a few types of autoimmune disease (such as rheumatic fever), a virus or infection with bacteria triggers an immune response and the antibodies or T-cells attack normal cells because some part of their structure resembles a part of the infecting microorganism.
Autoimmune disorders fall into two general categories: those that damage many organs (systemic autoimmune diseases) and those where only a single organ or tissue is directly damaged by the autoimmune process (localized). However, the distinctions become blurred as the effect of localized autoimmune disorders frequently extends beyond the targeted tissues, indirectly affecting other body organs and systems.
Causes of Autoimmune Hepatitis
Autoimmune hepatitis occurs when the body's immune system, which ordinarily attacks viruses, bacteria and other pathogens, instead targets the liver. This attack on your liver can lead to chronic inflammation and serious damage to liver cells. Just why the body turns against itself is unclear, but researchers think autoimmune hepatitis could be caused by an interaction between several risk factors, such as infections, medications and a genetic predisposition.
Risk factors
Factors that may increase your risk of autoimmune hepatitis include:
- Being female Although both men and women can develop autoimmune hepatitis, the disease is far more common in women.
- AgeType 1 autoimmune hepatitis can occur at any age. Type 2 primarily affects young girls.
- A history of certain infections Autoimmune hepatitis may develop after a bacterial or viral infection.
- Use of certain medications Certain medications, such as the antibiotic minocycline and the cholesterol medication atorvastatin (Lipitor) have been linked to autoimmune hepatitis.
- HeredityEvidence suggests that a predisposition to autoimmune hepatitis may run in families.
Signs and symptoms of autoimmune hepatitis can range from minor to severe and may come on suddenly or develop over time. Some people have few, if any, problems in the early stages of the disease, whereas others experience signs and symptoms that may include:
- Fatigue
- Abdominal discomfort
- Joint pain
- Itching (pruritus)
- Yellowing of the skin and whites of the eyes (jaundice)
- An enlarged liver
- Abnormal blood vessels on the skin (spider angiomas)
- Nausea and vomiting
Make an appointment with your doctor if you have any signs or symptoms that worry you.
Complications
Autoimmune hepatitis may be associated with a variety of other autoimmune diseases, including:
- Pernicious anemia Associated with a number of autoimmune disorders, pernicious anemia occurs when a lack of vitamin B-12 interferes with your body's ability to form red blood cells.
- Hemolytic anemia In this type of anemia, your immune system attacks and breaks down red blood cells faster than your bone marrow can replace them.
- Thrombocytopenic purpura Platelets are blood cells that help your blood clot. In thrombocytopenic purpura, your immune system attacks and destroys these cells, leading to easy bruising and bleeding.
- Ulcerative colitis This inflammatory bowel disease can cause severe bouts of watery or bloody diarrhea and abdominal pain.
- Autoimmune thyroiditis (Hashimoto's thyroiditis) In this condition, the immune system attacks the thyroid gland.
- Rheumatoid arthritis Another autoimmune disease, rheumatoid arthritis occurs when the immune system attacks the lining of your joints, leading to stiffness, pain, swelling, and sometimes deformity and disability.
- Celiac disease This disease causes an abnormal reaction to gluten, a protein found in most grains. Eating gluten sets off an immune response that damages the small intestine.
Tests and diagnosis
Tests and procedures used to diagnose autoimmune hepatitis include:
- Blood tests Testing a sample of your blood for antibodies can distinguish autoimmune hepatitis from viral hepatitis and other disorders with similar symptoms. Antibody tests also help pinpoint the type of autoimmune hepatitis you have.
- Liver biopsy Doctors perform a liver biopsy to confirm the diagnosis and to determine the degree and type of liver damage. During the procedure, a small amount of liver tissue is removed, using a thin needle that's passed into your liver through a small incision in your skin. The sample is then sent to a laboratory for analysis.
The goal in treating autoimmune hepatitis is to slow or stop your body's immune system from attacking your liver. This may help slow the progress of the disease. Medications to control your immune system (immunosuppressants) Medications used to treat autoimmune hepatitis include:
- PrednisoneDoctors usually recommend an initial high dose of the corticosteroid drug prednisone for people with autoimmune hepatitis. As soon as signs and symptoms improve, the medication is reduced to the lowest possible dose that controls the disease. Most people need to continue taking the prednisone for years and some people for life. Although you may experience remission a few years after starting treatment, the disease usually returns when the drug is discontinued.
Prednisone, especially when taken long term, can cause a wide range of serious side effects, including diabetes, thinning bones (osteoporosis), broken bones (osteonecrosis), high blood pressure, glaucoma and weight gain. - Azathioprine (Imuran) Azathioprine, another immunosuppressant medication, is sometimes used along with prednisone. Using both medications may reduce the dosage of prednisone needed, reducing its side effects. Side effects of azathioprine may include difficulty fighting infections and nausea. Rare side effects include liver damage, pancreas inflammation (pancreatitis) and cancer.
- Other immunosuppressants If you don't respond to prednisone or azathioprine, your doctor may prescribe stronger immunosuppressants, such as cyclosporine (Sandimmune) or tacrolimus (Prograf).
My Sick Liver
